Rewiring the Resilient Brain: A Comprehensive Guide to Transcranial Magnetic Stimulation (TMS) in Phoenix

Introduction: The Silent Crisis of Treatment Resistance
In the sprawling healthcare landscape of Phoenix and the West Valley, a silent crisis pervades the lives of thousands of residents. It is the crisis of the "medication merry-go-round"—the exhausting, often demoralizing cycle of trying one antidepressant after another, only to find that relief remains elusive. For decades, the standard of care for Major Depressive Disorder (MDD) has been pharmacological: a trial-and-error process of prescribing Selective Serotonin Reuptake Inhibitors (SSRIs) or Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs). While these medications are lifesaving for many, the STAR*D study—a landmark clinical trial—revealed a sobering reality: remission rates drop precipitously with each subsequent medication trial. By the time a patient has failed two medications, the likelihood of success with a third is discouragingly low.
This state of "Treatment-Resistant Depression" (TRD) is not merely a clinical classification; it is a lived experience of deepening despair, often compounded by the systemic side effects of oral medications, such as weight gain, sexual dysfunction, and emotional blunting. Patients begin to believe their depression is untreatable. However, at Trinity Integrated Medicine, we operate on a fundamental truth backed by neuroscience: the failure of medication is not a failure of the patient. It is often simply a failure of delivery. Oral medications flood the entire body to reach the brain. Transcranial Magnetic Stimulation (TMS) changes the paradigm entirely, bypassing the bloodstream to speak directly to the brain’s electrical circuitry.
The Neurobiology of Hope: How TMS Works
To understand the transformative potential of TMS, one must first understand the depressed brain not as "chemically imbalanced," but as "electrically disconnected." Advanced neuroimaging studies, including fMRI and PET scans, have consistently identified specific biomarkers associated with severe depression. The most significant finding is hypoactivity (reduced blood flow and glucose metabolism) in the Dorsolateral Prefrontal Cortex (DLPFC).
The DLPFC: The CEO of the Brain
The DLPFC serves as the brain's executive command center. It is responsible for mood regulation, decision-making, working memory, and the suppression of negative emotional responses generated by deeper, more primitive brain structures like the amygdala. In a healthy brain, the DLPFC exerts a "top-down" control, dampening fear and sadness. In a depressed brain, the DLPFC is sluggish, essentially asleep at the wheel. Consequently, the amygdala—the brain's fear center—becomes hyperactive, locking the patient in a state of chronic stress, anxiety, and low mood.3
Mechanism of Action: Electromagnetic Induction
TMS utilizes the principles of physics discovered by Michael Faraday to reactivate this dormant control center. The treatment involves placing a highly specialized electromagnetic coil against the scalp, precisely over the DLPFC.
- Pulse Generation: The device generates a rapidly alternating magnetic field, similar in strength to an MRI machine but highly focused.
- Induction: As these magnetic pulses pass non-invasively through the cranium, they induce a small electrical current in the neurons of the DLPFC.3
- Depolarization: This current causes the neurons to fire (depolarize), releasing neurotransmitters like serotonin, dopamine, and norepinephrine specifically in the relevant synapses, rather than systemically throughout the body.
- Neuroplasticity and Long-Term Potentiation (LTP): The true therapeutic power of TMS lies in repetition. Just as a muscle gets stronger with repetitive exercise, the neural circuits of the DLPFC strengthen through repetitive stimulation. This process, known as Long-Term Potentiation (LTP), physically strengthens the synaptic connections, "rewiring" the brain to regulate mood independently. Over a course of 4 to 6 weeks, the brain learns to stay active, leading to sustained remission for many patients.2
The Trinity Integrated Medicine Difference: Precision and Compassion
In Avondale and the greater Phoenix area, patients have choices for mental health care. However, Trinity Integrated Medicine offers a distinct advantage: the integration of advanced psychiatric technology within a comprehensive medical home. Led by Dr. Padma Aking, a board-certified psychiatrist with deep expertise in neuromodulation, our TMS program is not a standalone service but part of a holistic treatment ecosystem.7
Personalized Mapping and Motor Threshold
The effectiveness of TMS is entirely dependent on precision. During the initial "mapping" session, Dr. Aking and her clinical team do not use a one-size-fits-all approach. We utilize the patient's own physiology to calibrate the treatment.
- Finding the Motor Cortex: We first locate the motor cortex by administering single pulses to the scalp until we observe a visible twitch in the patient's thumb or hand.
- Determining Motor Threshold (MT): The minimum amount of energy required to produce this twitch is the "Motor Threshold." This is a critical safety and efficacy metric. It ensures that the treatment energy delivered to the prefrontal cortex is customized to the individual's unique conductivity and brain physiology, maximizing results while minimizing discomfort.6
The Patient Experience: What to Expect Day-by-Day
Fear of the unknown is a significant barrier to seeking advanced treatment. We believe in total transparency regarding the TMS experience. It is a rigorous but manageable commitment, designed to fit into a working life.
The Initial Consult and Mapping
The journey begins with a comprehensive psychiatric evaluation. Dr. Aking reviews the patient's history of medication trials, symptom severity, and safety contraindications (such as ferromagnetic metal implants). Once cleared, the patient undergoes the mapping process described above. This session typically lasts about 60 minutes.5
The Daily Treatment Routine
A standard course of FDA-cleared TMS therapy involves sessions five days a week for approximately six weeks, followed by a three-week taper period.
- Arrival: Patients arrive at our Avondale clinic. Because TMS requires no anesthesia or sedation, patients can drive themselves. There are no dietary restrictions.3
- The Session: The patient sits in a comfortable, spa-like treatment chair. The coil is positioned. When the machine is active, it produces a "tapping" sensation on the scalp and a clicking sound.
- Awake and Alert: Patients remain fully conscious. They can converse with our behavioral health coordinators, watch television, or listen to music. The lack of sedation is a massive advantage over treatments like Electroconvulsive Therapy (ECT).2
- Duration: Sessions typically last between 19 and 37 minutes, depending on whether standard rTMS or the accelerated intermittent Theta Burst Stimulation (iTBS) protocol is used.
- Immediate Return to Function: Upon completion, the patient can immediately return to work, school, or family responsibilities. There is no "recovery room" time needed.9
Safety Profile: A Clean Alternative to Systemic Medications
One of the most compelling arguments for TMS is its benign side effect profile. Antidepressants circulate through the entire blood supply, which is why they cause systemic issues like weight gain, dry mouth, constipation, and sexual libido loss. TMS is focal; it stays in the brain. Common Side Effects Scalp Discomfort: The most frequently reported side effect is mild to moderate scalp discomfort at the treatment site during stimulation. Crucially, this discomfort typically subsides after the first week as the scalp desensitizes to the sensation (see Cleveland Clinic side effects overview). While rare (occurring in less than 0.1% of patients), the most serious risk associated with TMS is a seizure (see clinical seizure risk discussion).
Common Side Effects
- Scalp Discomfort: The most frequently reported side effect is mild to moderate scalp discomfort at the treatment site during stimulation. This is caused by the contraction of superficial scalp muscles. Crucially, this discomfort typically subsides after the first week as the scalp desensitizes to the sensation.3
- Tension Headaches: Approximately one-third of patients may experience a mild tension headache following the first few sessions. These headaches are transient and generally respond well to over-the-counter analgesics.3
- No Systemic Effects: TMS does not cause weight gain, sexual dysfunction, memory loss, or drowsiness.3
Safety Protocols: Seizure Risk Mitigation
While rare (occurring in less than 0.1% of patients), the most serious risk associated with TMS is a seizure. This risk is comparable to or lower than the seizure risk associated with many common antidepressant medications (like Bupropion). At Trinity Integrated Medicine, we mitigate this risk through rigorous screening for pre-existing seizure disorders, alcohol withdrawal, or other neurological vulnerabilities. Our protocols ensure that patient safety is never compromised.3
Comparative Analysis: TMS vs. Other Modalities
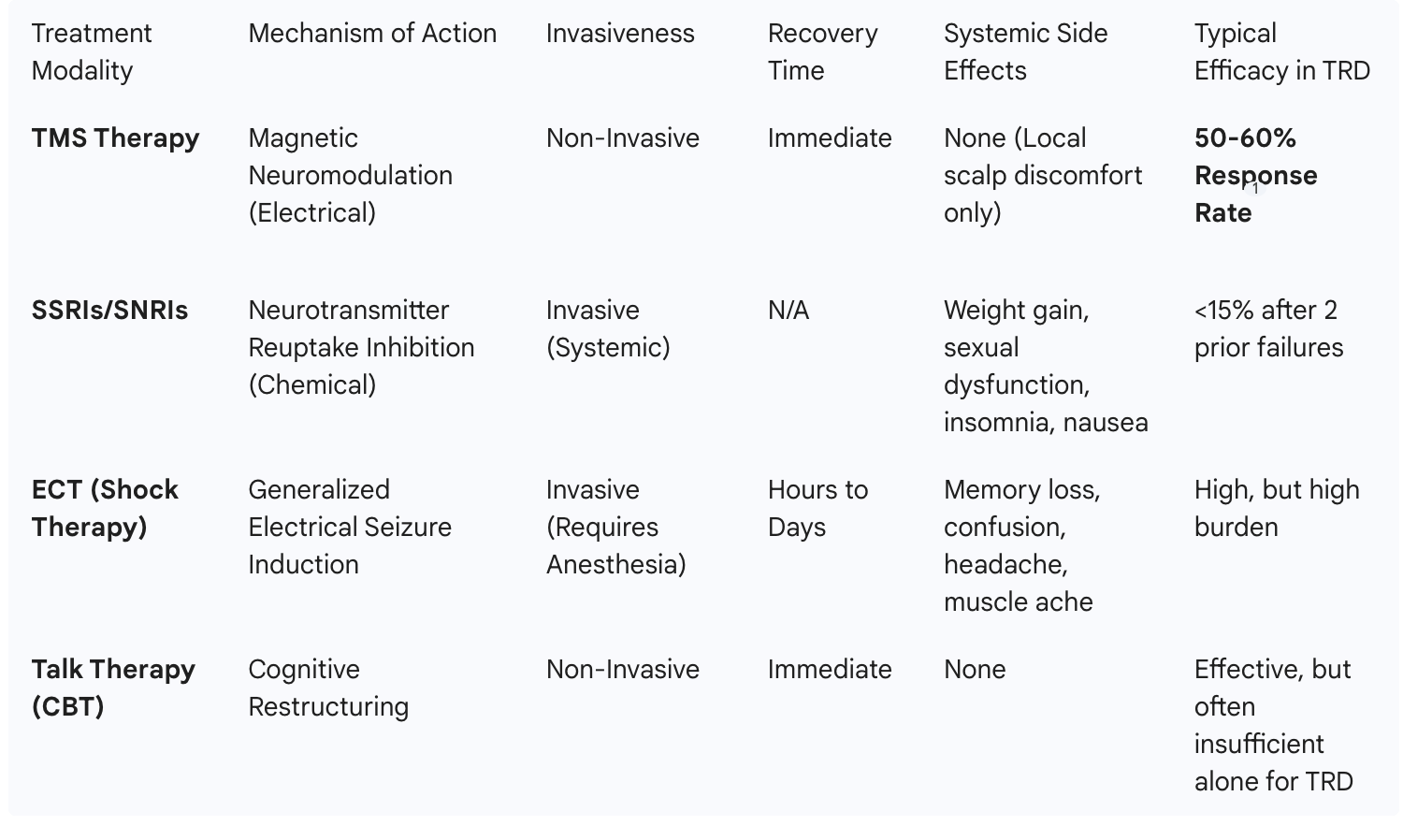
To assist patients in Phoenix in weighing their options, the following comparative analysis highlights the positioning of TMS relative to other standard-of-care options.
Beyond Depression: Treating the Anxious Brain
While the FDA clearance for TMS is primarily for Major Depressive Disorder (and more recently, OCD and smoking cessation), clinical experience and research suggest a broader utility. Anxiety and depression are highly comorbid; it is rare to find a patient with severe depression who does not also suffer from anxiety. The DLPFC—the target of TMS—is instrumental in regulating the emotional responses that drive anxiety. By strengthening the "brakes" of the brain (the prefrontal cortex), TMS can help dampen the "accelerator" (the amygdala), providing relief from the racing thoughts and physical tension of anxiety.1
At Trinity Integrated Medicine, Dr. Aking evaluates the patient's entire symptom cluster. For patients with "anxious depression," TMS can be a dual-purpose tool, calming the mind while lifting the mood. This integrated approach to symptom management is a hallmark of the Trinity philosophy.3
Navigating Insurance and Access in 2025
A common misconception is that TMS is an experimental or unaffordable "luxury" treatment. In 2025, this is factually incorrect. TMS is a standard-of-care treatment covered by most major insurance providers, including Medicare, Blue Cross Blue Shield, Cigna, UnitedHealthcare, and Aetna, provided the patient meets the criteria for Treatment-Resistant Depression.8
The Role of Trinity’s Administrative Team
Navigating "Prior Authorization" can be daunting for patients already struggling with low energy and motivation. Our administrative team in Avondale specializes in this advocacy. We gather the necessary documentation of prior medication trials and therapy history to build a compelling case for coverage. For patients with high deductibles or those without coverage, we offer transparent financial counseling to ensure that cost is not an insurmountable barrier to remission.8
Conclusion: A Future Without the Fog
For residents of Phoenix and Avondale, the message is clear: You do not have to settle for partial improvement. You do not have to accept that "this is as good as it gets." The brain is plastic; it is capable of change, growth, and healing, provided it receives the right stimulation.
TMS Therapy at Trinity Integrated Medicine represents the convergence of compassionate care and cutting-edge neuroscience. It is an opportunity to put down the pill bottle and pick up a solution that addresses the root cause of the dysfunction. If you have tried two or more medications without success, you owe it to yourself to explore the potential of magnetic stimulation.
Call Trinity Integrated Medicine today at (623) 873-0112 to schedule your TMS evaluation with Dr. Padma Aking.
- An Evidence-Based Look at TMS Therapy Reviews for Anxiety: Real Outcomes, Real Experiences
- Ketamine vs TMS: Understanding Your Mental Health Treatment Options.
- Does TMS Help Anxiety? An Honest Look at the Research
- Psychiatric Services - Trinity Medical Behavioral Health, accessed January 15, 2026, https://trinitymedical.care/psychiatric-services/
- Hope for Patients with Depression, OCD - Trinity Health, accessed January 15, 2026, https://www.trinityhealth.org/tms-offers-hope-to-patients-with-depression-ocd/
- TMS Therapy Pros & Cons: Honest Insights for Anyone Considering It
- Mental Health Care - Dr. Padma Aking - Trinity Integrated Medicine, accessed January 15, 2026, https://www.trinitymedicine.com/services/mental-health-care/
- Contact Us | Integrative Medicine Phoenix, AZ, accessed January 15, 2026, https://www.trinitymedicine.com/contact-us/
- What Does TMS Feel Like? Honest, Patient-Focused Guide
